19A177
Koebnerization of bone in a patient with multi-system sarcoidosis
Author(s)
Tahir Aziz1, Emma McDermott2, David Kane1, Ronan H Mullan1
Department(s)/Institutions
1. Department of Rheumatology, Tallaght University Hospital, Dublin 24 2. Department of Rheumatology. Our Lady's Hospital, Crumlin, Dublin 12
Introduction
Sarcoidosis is a multi system granulomatous disorder characterised by the presence of non-caseating granulomas in lung and extra thoracic tissues.
Aims/Background
Here we describe for the first time, the development of osseous sarcoidosis lesions following repeated minor nociceptive insults, consistent with sarcoidosis-induced Koebner phenomenon of bone.
Method
A 16 y/o patient with a previous history of thoracic and extra-thoracic sarcoidosis (biopsy-proven skin and nasopharyngeal involvement) successfully managed at Our Lady’s Hospital, Crumlin with adalibumab and oral corticosteroids, presented to the adolescent Transition Clinic at Tallaght University Hospital. He reporting new swelling on the shaft of the right little finger within 24 hours of a trivial subcutaneous knife cut but which had since persisted for months.
Results
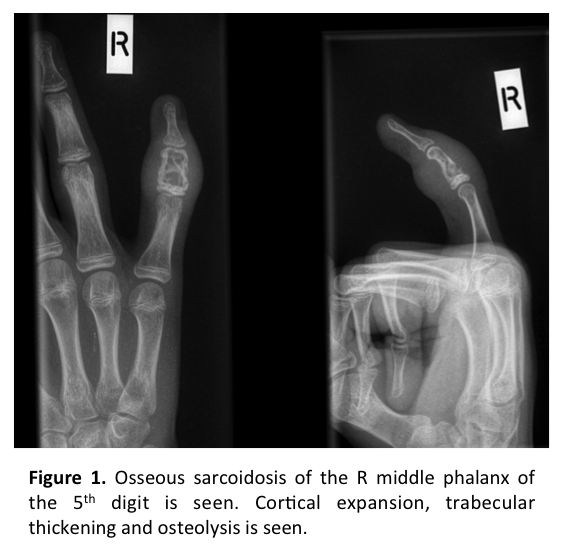
Examination revealed thickening of the right 5th middle phalanx with overlying violaceus discoloration of the skin. X-ray confirmed typical features of osseous sarcoidosis, with cortical expansion, osteolysis and trabecular thickening of bone (Fig 1). Three months later he presented with new persistant swelling of the distal phalanx of the right great toe after stubbing his toe on furniture. Clinical examination revealed swelling, with readiographic features consistent with new boney progression of osseous sarcoidosis of the great toe distal phalanx. Systemic features of sarcoidosis including pulmonary function tests, and serum markers have remained stable throughout. Dynamic technecium bone imaging and bone biomarker analysis are now awaited to assess bone disease activity, with a view to switching systemic sarcoidosis therapy.
Conclusions
Koebner phenomenon, also known as the Koebner or isomorphic response, refers to the development of skin lesions along previous lines of trauma, occurs in autoimmune diseases including psoriasis, vitiligo, lichen planus and sarcoidosis. Non-cutaneous Koebner lesions, including the oral mucosa, or at the site of internal organ scarring have been previously reported. This is the first documented case of ossesous Koebner phenomenon, in two separate bones following repeated minor trauma. Prior nociceptive stimulus leading to the development of new bone lesions, indicates the likely involvement of neurogenic pain pathways in granuloma formation. Elucidation of the pathological mechanisms of osseous sarcoidosis may lead to potential new therapeutic strategies to treat this debilitating condition.