18A101
Monitoring of lipids in patients on tocilizumab following introduction of ‘new subcutaneous tocilizumab progress chart’
Author(s)
Dr Katarzyna Nowak, Dr James Burns, Debbie Collins, Dr Claire Masih, Dr Gary Meenagh
Department(s)/Institutions
Rheumatology Department, Antirm Area Hospital, Northern Ireland
Introduction
Tocilizumab is a humanized monoclonal antibody that inhibits cytokine interleukin-6. The British Society for Rheumatology recommends lipid monitoring in patients receiving tocilizumab - fasting lipids at baseline and at 3 months into treatment.1
Aims/Background
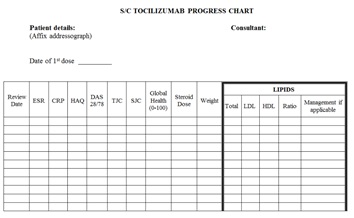
We carried out an audit looking at lipid monitoring in patients on tocilizumab between August 2016 and February 2017. It demonstrated that even if patients were having their lipid profile checked the results (when high) were not always acted upon. We have therefore identified a need for ‘new subcutaneous tocilizumab progress chart’ with the reminder to check lipids.
Method
We looked at all patients newly commenced on subcutaneous tocilizumab between October 2017 and April 2018. Eight patients were identified and retrospective data collection from medical charts was performed.
Results
The 'new subcutaneous tocilizumab progress chart’ was present in 75% of patients’ medical notes. 75% of patients had fasting lipids checked at baseline. The introduction of ‘new subcutaneous tocilizumab progress chart’ has increased the number of patients who had their lipids checked at 2-3 months into treatment from 50% to 75%. Furthermore, 100% of patients who were identified to have high cholesterol levels had appropriate plan of action recorded in their notes. The audit has also identified that those patients who did not have the new progress chart used in their notes had neither baseline nor repeat lipid profile done.
Conclusions
In summary, introduction of the ‘new subcutaneous tocilizumab progress chart’ improved lipid monitoring and management in patients newly commenced on subcutaneous tocilizumab therapy.
References:
1. Malaviya AP., Ledingham J. et al. “The 2013 BSR and BHPR guideline for the use of intravenous tocilizumab in the treatment of adult patients with rheumatoid arthritis”. Rheumatology 2014; 53:1344-1346